A selection of publications with educational value in
COPD
Most recently added articles listed first
-
Supranormal lung function: Prevalence, associated factors and clinical manifestations across the lifespan
Caspar Schiffers, Rosa Faner, Alina Ofenheimer, Owat Sunanta, Patricia Puchhammer, Tobias Mraz, Marie-Kathrin Breyer, Otto Chris Burghuber, Sylvia Hartl, Alvar Agustí, Robab Breyer-Kohansal (DOI: 10.1111/resp.14553)
onlinelibrary.wiley.com/doi/10.1111/resp.14553/full (September 2023)Comment by Dr Mark Lavercombe:
Supranormal spirometry values in an individual patient are of uncertain significance. In this report, authors evaluate an Austrian general population cohort to identify the prevalence of supranormal forced expiratory volume in one second (FEV1) and forced vital capacity (FVC). Multivariate regression analysis demonstrates that female sex, higher muscle mass, less diabetes, and fewer respiratory symptoms were all associated with supranormal spirometry results. Supranormal spirometry was associated with higher static lung volumes and lower specific airway resistance.20230822 -
Predictors of longitudinal changes in body weight, muscle and fat in patients with and ever-smokers at risk of COPD
Akio Yamazaki, Daisuke Kinose, Satoru Kawashima, Yoko Tsunoda, Yumiko Matsuo, Yasuki Uchida, Hiroaki Nakagawa, Masafumi Yamaguchi, Emiko Ogawa, Yasutaka Nakano (DOI: 10.1111/resp.14537)
onlinelibrary.wiley.com/doi/10.1111/resp.14537/full (September 2023)Comment by Dr Mark Lavercombe:
It is known that having Chronic Obstructive Pulmonary Disease results in increased energy expenditure, and that both weight loss and muscle loss are associated with poorer outcomes. In this study, the authors assessed annual body composition changes using computed tomography in a cohort of patients with COPD or at risk for COPD. Participants experienced an annual loss of weight and height, with no change in their body mass index, while decreased muscle mass and increased fat mass were noted over time. Muscle loss was most obvious in those with reduced lung function.20230719 -
Contribution of obesity to breathlessness in a large nationally representative sample of Australian adults
Yue Leon Guo, Maria R Ampon, Leanne M Poulos, Sharon R Davis, Brett G Toelle, Guy B Marks, Helen K Reddel
(DOI: 10.1111/resp.14400)
onlinelibrary.wiley.com/doi/10.1111/resp.14400/full (April 2023)Comment by Dr Mark Lavercombe:
The clinical experience of investigating and managing dyspnoea in patients with obesity is often challenging: it can be hard to know how much a particular patient's dyspnoea relates to their body habitus and how much to underlying cardiopulmonary dysfunction. This study estimates the contribution of obesity to breathlessness using the estimated population attributable fraction (PAF). In almost ten thousand survey respondents, and after adjusting for common comorbid adjusting variables, the estimated PAF ranged between 20-25%. This finding has significant implications for health planning and medical education in light of increasing obesity rates worldwide.20230305 
(Figure 2 of 10.1111/resp. 14222)
(Click image to enlarge)
(Figure 2 of 10.1111/resp. 14223)
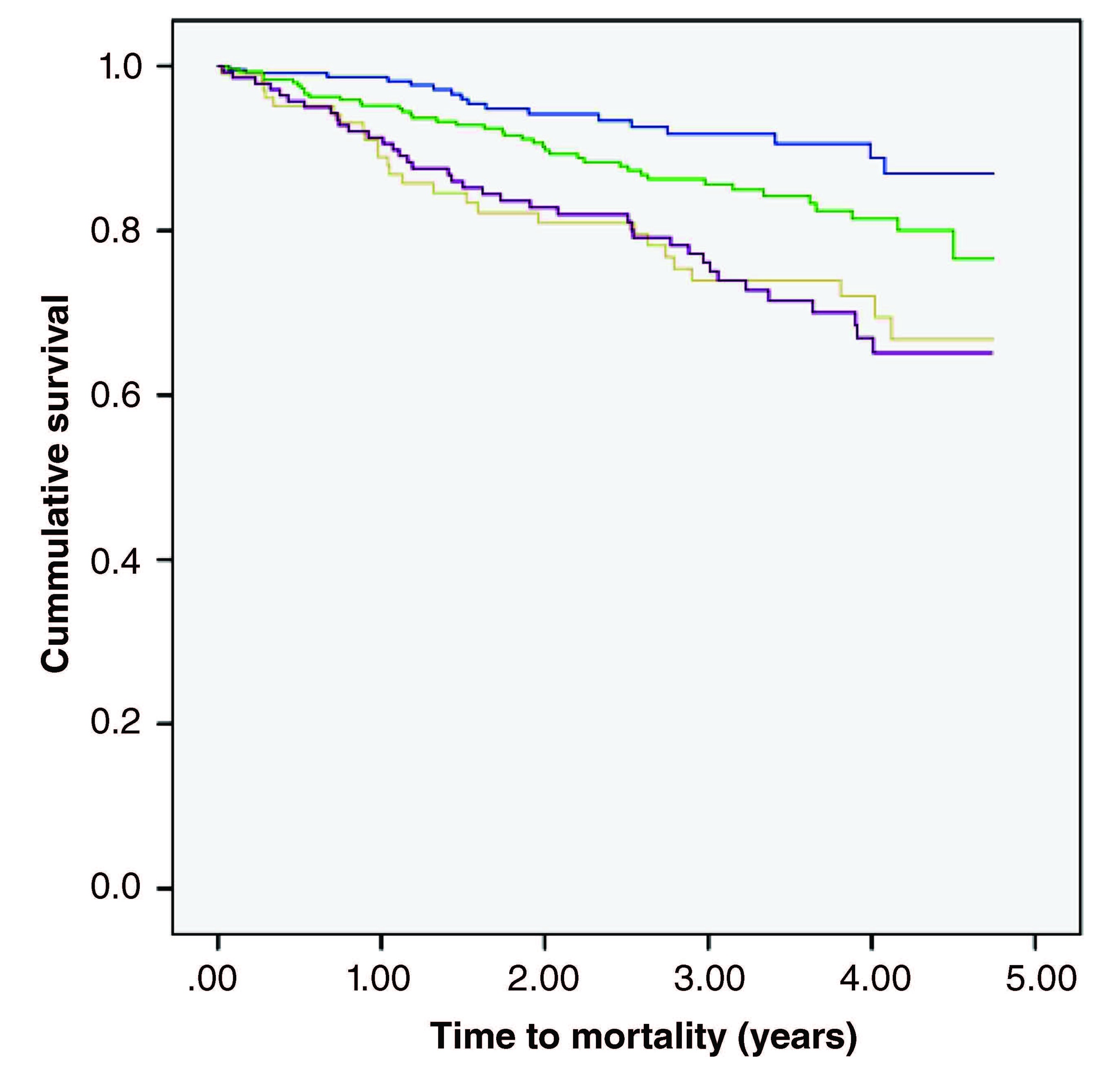
(Click image to enlarge)The HUNT study: Association of comorbidity clusters with long-term survival and incidence of exacerbation in a population-based Norwegian COPD cohort Sigrid Anna Aalberg Vikjord, Ben Michael Brumpton, Xiao-Mei Mai, Solfrid Romundstad, Arnulf Langhammer, Lowie Vanfleteren (DOI: 10.1111/resp.14222)
onlinelibrary.wiley.com/doi/10.1111/resp.14222/full (Apr 2022)Chest CT-assessed comorbidities and all-cause mortality risk in COPD patients in the BODE cohort Ana Ezponda, Ciro Casanova, Miguel Divo, Marta Marín-Oto, Carlos Cabrera, Jose M Marín, Gorka Bastarrika, Víctor Pinto-Plata, Ángela Martin-Palmero, Francesca Polverino, Bartolome R Celli, Juan P de Torres (DOI: 10.1111/resp.14223)
onlinelibrary.wiley.com/doi/10.1111/resp.14223/full (Apr 2022)Comment by Dr Mark Lavercombe:
In Respirology issue 27.4, there are two papers that examine the role of comorbidities in phenotyping patients with chronic obstructive pulmonary disease (COPD). Vikjord et al followed a cohort of patients for up to 25 years, and were able to cluster patients into groups with similar comorbidity profiles. Their 'psychological' and 'cachectic' clusters had significantly higher all-cause mortality than their 'less comorbidity' cluster. Further, Ezponda et al examined chest computed tomography (CT) findings in their COPD cohort and found that coronary artery calcium, bronchiectasis and low psoas muscle density were independently associated with all-cause mortality, features they term the 'CT-comorbidome'. Taken together, these papers provide new data that might help guide phenotyping in patients with COPD.20220324-
The needs and wellbeing of severe asthma and COPD carers: A cross-sectional study
Eleanor C Majellano, Vanessa L Clark, Peter G Gibson, Juliet M Foster, Vanessa M McDonald
onlinelibrary.wiley.com/doi/10.1111/resp.14167/full (Feb 2022)Comment by Dr Mark Lavercombe:
Caring for a patient with chronic medical conditions can be a significant burden for caregivers, and this study examines the degree and nature of those burdens in carers of patients with severe asthma and COPD. Although limited by its relatively homogeneous sample, the authors present important data that illustrate the physical and psychosocial impacts on caregivers. Further, the similarity between the impacts of caregiving in severe asthma when compared with carers of COPD patients suggests a potential unmet need for carers of severe asthma patients.20220202 -
Impact of early life exposures on COPD in adulthood: A systematic review and meta-analysis
Pengfei Duan, Yao Wang, Rongqing Lin, Yiming Zeng, Chengshui Chen, Li Yang, Minghui Yue, Shan Zhong, Yun Wang, Qingying Zhan (DOI: 10.1111/resp.14144)
onlinelibrary.wiley.com/doi/10.1111/resp.14144/full (Sep 2021)Comment by Dr Mark Lavercombe:
This systematic review and meta-analysis examines the impact of early life exposures to risk factors and the subsequent development of COPD as an adult. Using 30 studies with almost 800 000 participants, the authors find significant associations between childhood serious respiratory infections, pneumonia and bronchitis, asthma, maternal smoking, low birth weight and childhood maltreatment. This study suggests a potential role for addressing these exposures in children for COPD prevention.20211122 -
Underuse of beta-blockers by patients with COPD and co-morbid acute coronary syndrome: A nationwide follow-up study in New Zealand Lianne Parkin, Joshua Quon, Katrina Sharples, David Barson and Jack Dummer (DOI: 10.1111/resp.13662)
onlinelibrary.wiley.com/doi/10.1111/resp.13662/full (Feb 2020)Comment by Dr Mark Lavercombe:
In this nationwide study of 83425 patients with COPD, of whom 2637 had one or more acute coronary syndrome events during follow-up, low rates of beta-blocker prescription is found. This finding is especially pronounced in those with very severe COPD despite international guidelines recommending the use of beta-blockers in patients with coronary ischaemia and COPD.20200203 -
Increased risk of major adverse cardiac events following the onset of acute exacerbations of COPD Mette Reilev, Anton Pottegard, Jesper Lykkegaard, Jens Søndergaard, Truls S Ingebrigtsen and Jesper Hallas (DOI: 10.1111/resp.13575)
onlinelibrary.wiley.com/doi/10.1111/resp.13575/full (Dec 2019)Comment by Dr Mark Lavercombe:
Multiple studies have demonstrated an increase in cardiovascular outcomes in patients with COPD, and treatment with cardiac medications in patients with AECOPD has also been investigated. This large study demonstrates that adverse cardiac outcomes are markedly increased in patients with AECOPD, and especially in those who require hospitalisation.20191113 -
Nasal high-flow therapy compared with non-invasive ventilation in COPD patients with chronic respiratory failure: A randomized controlled cross-over trial Steven Mckinstry, Joseph Singer, Jan Pieter Baarsma, Mark Weatherall, Richard Beasley and James Fingleton (DOI: 10.1111/resp.13575)
onlinelibrary.wiley.com/doi/10.1111/resp.13575/full (May 2019)Comment by Dr Mark Lavercombe:
Two papers published in Respirology Issue 24.11 (November 2019) consider the role of Nasal High Flow (NHF) therapy in patients with COPD. In this paper, NHF is compared with NIV (untitrated) in stable COPD patients with chronic hypercapnic respiratory failure. Patients found NHF easier to use and more comfortable, although NIV had more marginally more effect on PtCO2 levels.20191015 -
Nasal high flow does not improve exercise tolerance in COPD patients recovering from acute exacerbation: A randomized crossover study Guillaume Prieur, Clement Medrinal, Yann Combret, Elise Dupuis Lozeron, Tristan Bonnevie, Francis-Edouard Gravier, Jean Quieffin, Bouchra Lamia, Jean-Christian Borel and Gregory Reychler (DOI: 10.1111/resp.13664)
onlinelibrary.wiley.com/doi/10.1111/resp.13664/full (Apr 2018)Comment by Dr Mark Lavercombe:
Two papers published in Respirology Issue 24.11 (November 2019) consider the role of Nasal High Flow (NHF) therapy in patients with COPD. In this paper, addition of NHF with air (or oxygen for those requiring LTOT) during high intensity exercise did not improve endurance during pulmonary rehabilitation. Several potential explanations for discordance with prior studies are considered.20191015 -
Exertional hypoxemia is more severe in fibrotic interstitial lung disease than in COPD Jean P Du Plessis, Senan Fernandes, Rakin Jamal, Pat Camp, Kerri Johannson, Michele Schaeffer, Pearce G Wilcox, Jordan A Guenette and Christopher J Ryerson (DOI: 10.1111/resp.13226)
onlinelibrary.wiley.com/doi/10.1111/resp.13226/full (Apr 2018)Comment by Dr Mark Lavercombe:
Clinicians have long relied on extrapolation of data from COPD studies to inform decision making around oxygen supplementation in patients with other chronic lung diseases. This study demonstrates a difference between patients with fibrotic ILDs and COPD in the degree of exertional oxygen desaturation, raising important questions about the appropriateness of extrapolation.20180320 -
Year in review 2017: Chronic obstructive pulmonary disease and asthma Melissa J Benton, Tow Keang Lim, Fanny W S Ko, Keiko Kan-o, Judith C W Mak (DOI: 10.1111/resp.13285)
onlinelibrary.wiley.com/doi/10.1111/resp.13285/full (Mar 2018)20180313 -
Small airway disease: A different phenotype of early stage COPD associated with biomass smoke exposure Dongxing Zhao, Yumin Zhou, Changbin Jiang, Zhuxiang Zhao, Fang He And Pixin Ran (DOI: 10.1111/resp.13176)
onlinelibrary.wiley.com/doi/10.1111/resp.13176/full (Feb 2018)Comment by Dr Mark Lavercombe:
The authors of this paper describe the distinct pathology, physiology and radiology findings in a cohort of patients with biomass smoke exposure associated COPD compared with COPD related to cigarette smoking. They provide evidence of a distinct COPD phenotype that warrants further study.20180126 -
History of pulmonary tuberculosis affects the severity and clinical
outcomes of COPD Hye Jung Park, Min Kwang Byun, Hyung Jung Kim, Chul Min Ahn, Deog Kyeom Kim, Yu Il Kim, Jin Young Oh, Hyoung Kyu Yoon, Kwang-Ha Yoo and Ki Suck Jung (DOI: 10.1111/resp.13147)
onlinelibrary.wiley.com/doi/10.1111/resp.13147/full (Jan 2018)Comment by Dr Mark Lavercombe:
The authors of this paper describe a cohort of patients with COPD who were stratified based on self-report of prior history of tuberculosis infection. Patients who admitted to prior Tb had more severe symptoms of COPD, poorer lung function and more frequent exacerbations. This difference was noted despite a lower prevalence of ongoing smoking in the tuberculosis group.20171208 -
Spirometry reference values for population aged 7–80 years in China: Jingzhou Zhang, Xiao Hu and Guangliang Shan (DOI: 10.1111/resp.13118)
onlinelibrary.wiley.com/doi/10.1111/resp.13118/full (Nov 2017)Comment by Dr Mark Lavercombe:
Using data from the China National Health Survey 2012–2015, the authors of this paper propose spirometry prediction equations for a general Chinese population aged 7–80 years. Their equations compare favourably to those developed in more heterogeneous cohorts.20171027 - Home-based telerehabilitation via real-time videoconferencing improves endurance exercise capacity in patients with COPD: The randomized controlled TeleR Study Ling Ling Y Tsai, Renae J McNamara, Chloe Moddel, Jennifer A Alison, David K McKenzie & Zoe J McKeough 10.1111/resp.12966 (May 2017)

The respiratory telerehabilitation (TeleR) trial team from Sydney, Australia
(Click image to enlarge)Despite the clear health benefits in COPD patients, participation in pulmonary rehabilitation is variable with potential barriers including reduced mobility, lack of transport or travel costs. This randomised controlled trial evaluates home-based telerehabilitation compared with usual care and finds improved endurance exercise capacity and self-efficacy in the treatment group. Telerehabilitation might be an alternative option for pulmonary rehabilitation in those unable to attend centralised programmes. Table 3 presents outcomes for special consideration.
20170415 -
Frailty is common and strongly associated with dyspnoea severity in fibrotic interstitial lung disease, Kathryn M Milne, Joanne M Kwan, Sabina Guler, Tiffany A Winstone, Angela Le, Nasreen Khalil, Pat G Camp, Pearce G Wilcox & Christopher J Ryerson
10.1111/resp.12944 (May 2017)Prognosis in patients with fibrotic interstitial lung diseases can vary significantly. In this study, the authors demonstrate that Frailty is highly prevalent in a cohort of patients with fibrotic ILD and strongly associated with dyspnoea severity. The authors propose a potential role for frailty assessment in identifying patients at risk of complications from invasive procedures or medical therapies, and/or mortality.
20170415 Pulmonary Rehabilitation Guidelines for Australia and New Zealand Jennifer A Alison, Zoe J McKeough, Kylie Johnston, Renae J McNamara, Lissa M Spencer, Sue C Jenkins, Catherine J Hill, Vanessa M McDonald, Peter Frith, Paul Cafarella, Michelle Brooke, Helen L Cameron-Tucker, Sarah Candy, Nola Cecins, Andrew S L Chan, Marita T Dale, Leona M Dowman, Catherine Granger, Simon Halloran, Peter Jung, Annemarie L Lee, Regina Leung, Tamara Matulick, Christian Osadnik, Mary Roberts, James Walsh, Sally Wootton, Anne E Holland, on behalf of the Lung Foundation Australia and the Thoracic Society of Australia and New Zealand 10.1111/resp.13025 (Apr 2017)
The aim of these Guidelines is to provide evidence-based recommendations for the practice of pulmonary rehabilitation (PR) specific to Australian and New Zealand healthcare contexts.
These first-ever pulmonary rehabilitation Guidelines for Australia and New Zealand were launched (24-28 March 2017) at the TSANZSRS Annual Scientific Meeting in Canberra, Australia (24-28 March 2017), and were drawn up following a systematic review of over 275 clinical trials.
The Guidelines recommend that all COPD patients should be offered pulmonary rehabilitation regardless of their disease severity.
See the full Editorial for these important Guidelines at onlinelibrary.wiley.com/doi/10.1111/resp.13039/full
20170329Global Strategy for the Diagnosis, Management, and Prevention of Chronic Obstructive Lung Disease 2017 Report Claus F Vogelmeier, Gerard J Criner, Fernando J Martinez, Antonio Anzueto, Peter J Barnes, Jean Bourbeau, Bartolome R Celli, Rongchang Chen, Marc Decramer, Leonardo M Fabbri, Peter Frith, David M G Halpin, M Victorina López Varela, Masaharu Nishimura, Nicolas Roche, Roberto Rodriguez-Roisin, Don D Sin, Dave Singh, Robert Stockley, Jørgen Vestbo, Jadwiga A Wedzicha and Alvar Agusti 10.1111/resp.13012 (Apr 2017)
This Executive Summary focuses primarily on the revised and novel parts of the document, including:
- the assessment of COPD has been refined to separate the spirometric assessment from symptom evaluation. ABCD groups are now proposed to be derived exclusively from patient symptoms and their history of exacerbations;
- for each of the groups A to D, escalation strategies for pharmacological treatments are proposed;
- the concept of de-escalation of therapy is introduced in the treatment assessment scheme;
- nonpharmacologic therapies are comprehensively presented;
- the importance of comorbid conditions in managing COPD is reviewed.
20170205-
Prevalence and outcomes of diaphragmatic dysfunction assessed by ultrasound technology during acute exacerbation of COPD: A pilot study Federico Antenora, Riccardo Fantini, Andrea Iattoni, Ivana Castaniere, Antonia Sdanganelli, Francesco Livrieri, Roberto Tonelli, Stefano Zona, Marco Monelli, Enrico M Clini & Alessandro Marchioni DOI: 10.1111/resp.12916
onlinelibrary.wiley.com/doi/10.1111/resp.12916/full (Feb 2017)Comment by Dr Mark Lavercombe:
The indications for thoracic ultrasonography continue to expand, and this study suggests another indication. Diaphragmatic dysfunction found on ultrasound on admission in patients with acute hypercapnic exacerbations of COPD is identified as a risk factor for failure of NIV, duration of mechanical ventilation and short-term mortality. This non-invasive test might help clinicians identify patients at risk of failing standard care.20170131 -
Role of BMI, airflow obstruction, St George's Respiratory Questionnaire and age index in prognostication of Asian COPD. Chan et al. (resp12877/RES-16-062.R2)
onlinelibrary.wiley.com/doi/10.1111/resp.12877/full (Jan 2017)Comment by Dr Mark Lavercombe:
This study identifies important risk factors for mortality in Asian patients with COPD, and develops a prognosis model that is easy to use. Further validation studies will be required to assess its utility.20161220 -
Etiology of bronchiectasis in adults: a systematic literature review Gao et al. (resp. 12832/ RES-15-983.R2)
onlinelibrary.wiley.com/doi/10.1111/resp.12832/full (Jun 2016)Comment by Dr Mark Lavercombe:
This systematic review identifies regional variations in the underlying aetiologies for non-CF bronchiectasis, which is important to consider when evaluating the applicability of the bronchiectasis literature. It also provides an evidence base for the clinical workup of these patients leading to a change in management.20161021 Increasing awareness of sex differences in airway diseases. Raghavan and Jain.
onlinelibrary.wiley.com/doi/10.1111/resp.12702/abstract (Dec 2015)20160819Insulin resistance is associated with skeletal muscle weakness in COPD. Wells et al.
onlinelibrary.wiley.com/doi/10.1111/resp.12716/abstract (Dec 2015)20160819Differences in baseline factors and survival between normocapnia, compensated respiratory acidosis and decompensated respiratory acidosis in COPD exacerbation: A pilot study. Lun et al.
onlinelibrary.wiley.com/doi/10.1111/resp.12652/abstract (Oct 2015)20160819Efficacy and tolerability of budesonide/formoterol added to tiotropium compared with tiotropium alone in patients with severe or very severe COPD: A randomized, multicentre study in East Asia. Lee et al.
onlinelibrary.wiley.com/doi/10.1111/resp.12646/abstract (Sep 2015)20160819Mother's smoking and complex lung function of offspring in middle age: A cohort study from childhood. Perret et al.
onlinelibrary.wiley.com/doi/10.1111/resp.12750/abstract (Mar 2016)
(FREE access: Editor's Choice)20160819